A patient support program (PSP) is a structured set of services — typically funded by a pharmaceutical company — that helps patients access, afford, and adhere to prescribed therapies throughout their treatment journey. Services commonly include enrollment and onboarding assistance, insurance navigation and prior authorization support, financial assistance and co-pay programs, medication adherence tools, disease education, and emotional and lifestyle support.
PSPs have become business-critical in pharma because they directly address the gap between prescribing and outcomes. The global PSP market was valued at approximately USD 21.8 billion in 2024 and is projected to grow at a 17.1% CAGR through 2034, driven by the shift toward specialty and high-cost therapies where patient support directly impacts adherence, persistence, and commercial performance. For pharmaceutical executives, PSPs are now embedded into launch planning from day one — particularly for oncology, immunology, and rare disease therapies where treatment complexity and cost create significant barriers to access.
For digital health startups and platforms, PSPs offer a scalable frontier to deploy modular, patient-centric solutions that integrate into broader care ecosystems. These programs are fertile ground for innovation around automation, engagement, and personalization.
Why Patient Support Programs Are Business-Critical in Pharma
The value of PSPs extends beyond patient satisfaction or brand goodwill. They directly address operational and clinical inefficiencies by:
- Reducing treatment delays due to insurance barriers, missing documentation, or lack of awareness
- Improving adherence and persistence by engaging patients at key points in their journey
- Enhancing therapeutic outcomes through education, monitoring, and coaching
- Providing emotional and logistical support during complex or chronic treatments
- Generating real-world insights that inform commercial, medical, and R&D strategies
Simply put, a well-designed PSP can influence both the top and bottom line for pharmaceutical brands.
The WHO's global report on chronic disease management underscores that improving medication adherence may have a greater population health impact than any improvement in specific medical treatments — making PSPs one of pharma's highest-leverage investments.
Core Components of an Effective PSP
While the structure of PSPs varies by product type and patient population, successful programs tend to include the following pillars:
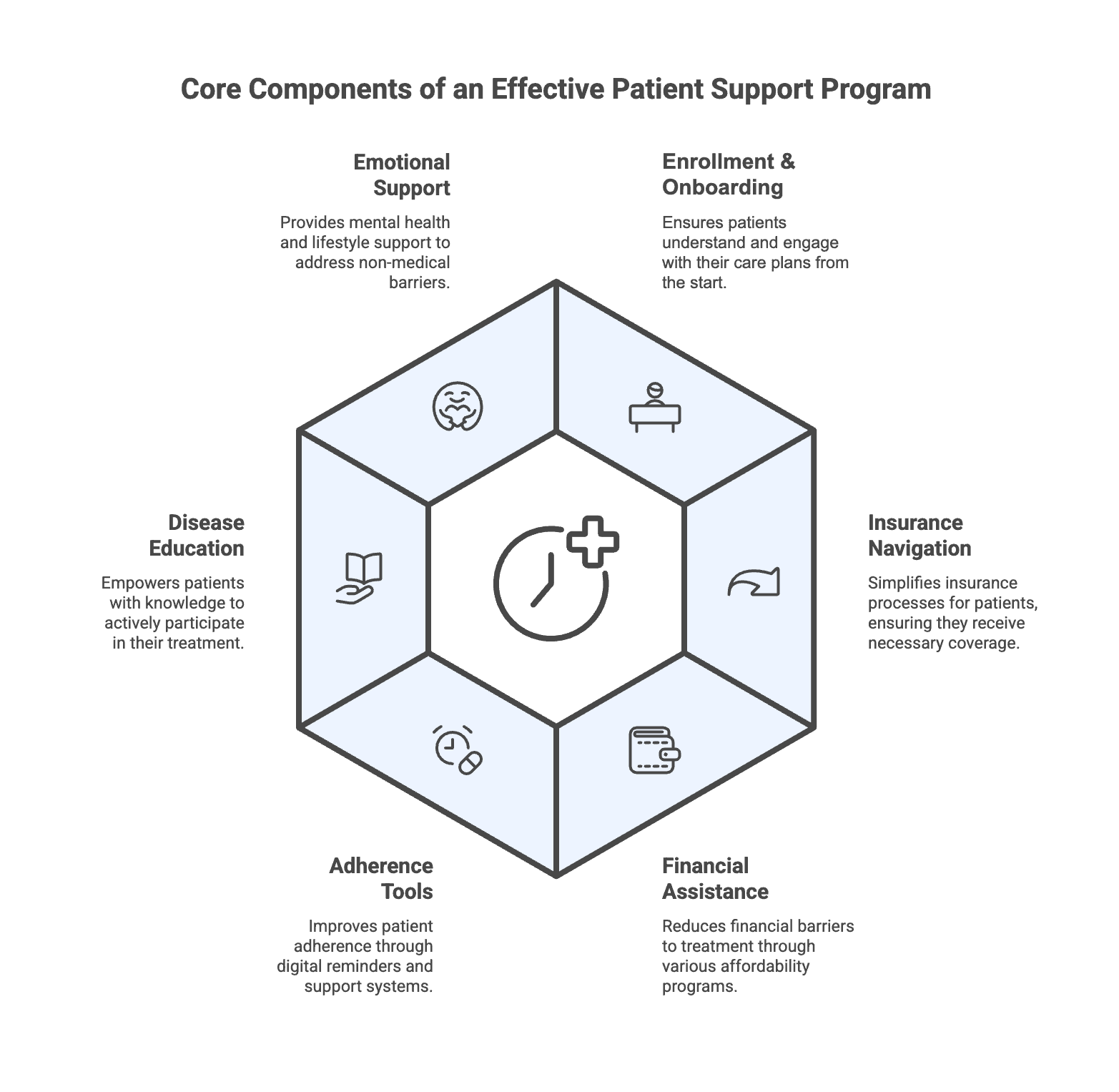
1. Enrollment & Onboarding
Support services to help patients complete enrollment forms, obtain prior authorizations, and understand their care plans. Early engagement ensures that patients don’t abandon treatment before it even begins.
2. Insurance Navigation & Reimbursement Support
Many patients are unfamiliar with insurance workflows. PSPs simplify this through dedicated teams or automated tools that manage prior authorizations, benefits verification, appeals processes, and co-pay eligibility.
3. Financial Assistance & Affordability Programs
High out-of-pocket costs are a leading cause of non-initiation. PSPs often include co-pay cards, patient assistance programs (PAPs), or connections to financial foundations to reduce cost-related abandonment.
4. Adherence Tools & Ongoing Engagement
Digital nudges, medication reminders, refill tracking, and live nurse support can drastically improve adherence. Some PSPs use AI or predictive analytics to flag patients at risk of drop-off. For a deeper look at where this is headed, see our analysis of how AI is transforming patient support programs in 2026, from predictive adherence models to automated care coordination.
5. Disease Education & Treatment Literacy
Many patients drop out simply due to fear or misunderstanding. Educational content—via SMS, email, apps, or HCP outreach—helps patients and caregivers become active participants in treatment.
6. Emotional and Lifestyle Support
PSPs that include mental health coaching, social support, or lifestyle planning (diet, mobility, sleep) address non-medical barriers to success. This humanized layer increases trust and satisfaction.
How Digital Health Platforms Are Redefining Patient Support Programs
Traditional PSPs were often fragmented, heavily reliant on call centers, and difficult to scale. Today, digital health innovators are reimagining PSPs through platform-based approaches:
- Self-service portals that empower patients to enroll, manage reminders, and track outcomes
- Automated onboarding workflows that speed up time to therapy
- Omnichannel engagement tools such as mobile apps, two-way SMS, emails, and IVR
- Dashboards and analytics tools for HCPs, pharma teams, and case managers
- EHR and CRM integrations that create a seamless experience across clinical and commercial workflows
Zelthy's patient support program platform is built on this digital-first model — shipping with AI agents for enrollment validation, adherence prediction, and call scheduling so teams focus on work that moves patient outcomes.
One Size Doesn’t Fit All: Customization Is Critical
No two therapies or patient populations are the same. That’s why successful PSPs require intentional design that aligns with:
- Therapeutic area and product complexity (e.g., chronic injectables vs. one-time treatments)
- Demographics and digital literacy (e.g., tech-savvy millennials vs. seniors)
- Channel and communication preferences (e.g., live nurse calls vs. automated SMS)
Pharma companies must avoid over-engineered, one-size-fits-all programs and instead prioritize modularity and patient segmentation.
Regulatory frameworks add another layer of variation; PSP design in the US emphasizes insurance navigation while EU programs focus on outcomes measurement and EFPIA compliance. Our US vs EU PSP comparison breaks down these differences in detail.
The FDA's Patient-Focused Drug Development guidance reinforces this principle, emphasizing that patient experience data should inform not just clinical development but also the support infrastructure around therapies.
Final Thoughts
As healthcare moves steadily toward value-based care models, where success is measured by patient outcomes rather than volume, PSPs will become even more vital.
- For pharma executives, PSPs should be embedded into early launch planning, especially for specialty drugs or rare disease therapies.
- For digital health founders, this space represents an opportunity to create API-first, outcomes-driven platforms that pharma can plug into with minimal friction.
Expect increased convergence of PSPs with digital therapeutics, remote patient monitoring, and AI-driven care coordination in the next wave.
Patient Support Programs have evolved from back-office support services into mission-critical engines for patient experience, adherence, and brand differentiation. In a crowded therapeutic market with rising pressure on real-world outcomes, PSPs are now central to pharma’s commercial success and digital health's platform opportunities.
Organizations that treat PSPs as strategic assets, rather than compliance checkboxes will be best positioned to lead in the next era of connected, patient-centric care.
Want to explore how Zelthy can transform your PSP operations? Book a demo. Contact us at connect@zelthy.com or send us a DM on LinkedIn for more information.
Frequently Asked Questions
What is a Patient Support Program (PSP)?
A Patient Support Program (PSP) is a structured suite of services developed by pharmaceutical companies to assist patients at every stage of their treatment journey — from initial prescription through long-term adherence. Services typically include medication access support, insurance navigation, financial assistance, disease education, digital engagement, and adherence monitoring. PSPs address clinical, commercial, and regulatory objectives simultaneously.
What are the core components of an effective PSP?
Effective PSPs are built around six pillars: (1) enrollment and onboarding support to prevent pre-treatment dropout; (2) insurance navigation and prior authorization management; (3) financial assistance and co-pay support; (4) adherence tools including digital reminders and nurse outreach; (5) disease education and treatment literacy programs; and (6) emotional and lifestyle support for patients managing chronic or complex therapies. Programs that address all six outperform those focused solely on access or financial aid.
Why are PSPs business-critical for pharmaceutical companies?
PSPs directly impact commercial performance by reducing prescription abandonment rates — which reach 30–40% for specialty medications — extending treatment duration, and protecting market share. Clinically, they address the 50% of patients who do not take medications as prescribed, contributing to $100–300 billion in avoidable annual healthcare costs. For specialty and rare disease therapies, a well-designed PSP can be the difference between a commercially successful launch and early market withdrawal.
How have digital platforms changed PSP delivery?
Digital platforms have transformed PSP delivery from call-center-dependent, fragmented operations to scalable, omnichannel engagement models. Self-service patient portals, automated onboarding workflows, ePRO and wearable integrations, and two-way SMS engagement reduce manual workload while improving patient experience. EHR and CRM integrations create continuity between clinical and commercial workflows. Digital-first PSPs also generate structured patient behavior data that supports real-world evidence generation and adherence analytics.
How should PSPs be customized for different patient populations?
PSP customization requires alignment with the therapy's complexity, the patient population's demographics, and preferred communication channels. A chronic injectable therapy for older patients requires different support — live nurse calls, simpler digital interfaces — than a one-time treatment for younger, tech-comfortable patients. Over-engineered one-size-fits-all programs consistently underperform compared to modular designs that allow patient segmentation and channel-specific personalization based on real enrollment and engagement data.
What role does real-world evidence play in PSPs?
PSPs are a primary source of real-world evidence (RWE) for pharmaceutical companies. Patient-reported outcomes, adherence rates, adverse events, and healthcare utilization data collected through PSP operations support health technology assessments, payer reimbursement negotiations, and post-market regulatory submissions. In EU markets particularly, the quality of RWE generated by PSPs increasingly influences market access decisions and value-based pricing discussions with national health authorities.
What is the difference between a PSP and a Patient Assistance Program (PAP)?
A Patient Assistance Program (PAP) is a specific type of financial aid program that provides free or discounted medications to patients who cannot afford them. A PSP is broader: it encompasses PAPs as one component but also includes insurance navigation, clinical case management, adherence monitoring, disease education, and digital engagement. PSPs serve both patients who face financial barriers and those who face clinical, logistical, or informational barriers to staying on therapy.


![AI Output Compliance Monitoring in Pharma: The Watch Layer [2026]](/_next/image?url=https%3A%2F%2Fhumble-friendship-ab99f71d93.media.strapiapp.com%2FAI_Compliance_in_Pharma_a76c884d28.png&w=3840&q=75)
